Sponsored content brought to you by
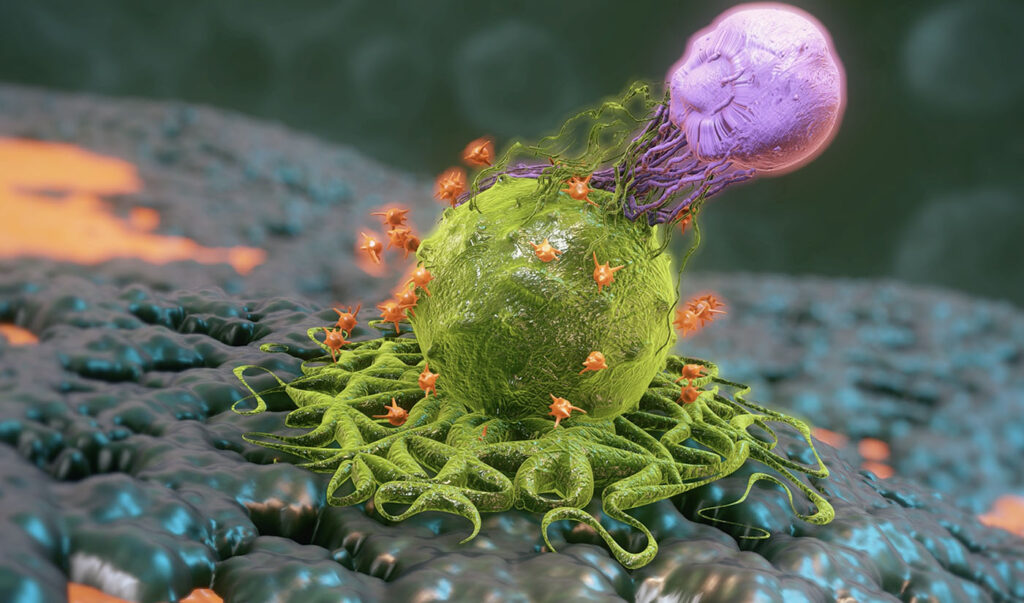
Chimeric antigen receptor T cell (CAR T) therapies have transformed the treatment of blood cancers, delivering durable responses in patients with limited options. But CAR T therapies are complex and require patient- specific manufacturing that is costly, time-consuming, and logistically demanding. Consequently, developers are turning to in vivo CAR T, which engineers therapeutic T cells directly inside the patient’s body.
“In vivo CAR T has taken the main stage as a very targeted, advanced gene therapy option,” says Annie Huang, senior manager of content marketing at GenScript ProBio. More than 100 biotech companies focused on cell therapy and mRNA technologies have entered the space, and several programs are expected to reach investigator-initiated trials (IITs) or advance toward Investigational New Drug (IND) applications within the next year.
From weeks to hours
Traditional ex vivo CAR T manufacturing begins by collecting a patient’s blood and isolating T cells. These cells are genetically modified—often using lentiviral vectors (LVVs)—to introduce the CAR construct, expanded in vitro, tested, and reinfused. The vein-to-vein process takes two to seven weeks, during which disease may progress, and it requires specialized facilities and rigorous quality controls.
In vivo CAR T streamlines this workflow. Instead of modifying cells outside the body, developers deliver a viral vector or lipid nanoparticle-formulated mRNA (mRNA-tLNP) carrying the CAR gene directly into the patient, enabling T cells to express the CAR in vivo. “Not only do you save time and money, but you reduce room for error by eliminating the need for cell culture,” Huang says. “With fewer steps, the in vivo CAR T production workflow is significantly optimized compared to ex vivo, which cuts down on time to therapy.”
To support this shift, ProBio integrates discovery, pharmacology, and chemistry, manufacturing, and controls (CMC) into a unified platform advancing LVV and mRNA-tLNP programs from sequence design to IND readiness.
Engineering around LVV complexity
Developing LVVs for in vivo use introduces technical and analytical challenges. In upstream processing, crude titers may decrease when modifying the VSV-G envelope plasmid or introducing plasmids encoding targeting antibodies.
Downstream, modified envelope proteins increase the risk of vector aggregation and demand tighter control of impurity profiles, including host-cell proteins (HCPs). Moreover, tailored analytical methods are required to characterize potency, safety, and quality attributes.
ProBio can move from sequence to the start of an IIT in roughly four months for LVV-based in vivo CAR T programs—an accelerated timeline designed to generate early clinical data to support future IND filings.
Nuances of using lipid nanoparticles
For CAR T therapy based on mRNA-tLNPs, surface ligands—commonly antibody fragments—guide delivery to specific immune cells.
As a newer modality, mRNA-tLNP brings distinct CMC hurdles. Antibody fragments often have low expression titers and complex purification requirements. Scaling from laboratory to clinical production presents additional technical barriers. The ratio of antibody to LNP must be optimized for each candidate, as it directly affects in vitro and in vivo efficacy.
Consequently, ProBio built a technology toolbox spanning plasmid design through mRNA-tLNP formulation. “We provide a one-stop shop—instead of the need to source antibodies from one company, plasmids from a different company, and then get LNP packaging from somewhere else,” Huang says. “We do it all through a consolidated platform.”
With that platform, ProBio produces capping efficiencies above 90% and mRNA yields up to 10 grams per liter. “Our production process improves yield and product purity, and we’re there every step of the way with quality control and assurance,” Huang notes. For mRNA-tLNP programs, ProBio estimates approximately five months from sequence to IIT initiation.
Building a regulatory bridge
IITs are emerging as an accelerated pathway for in vivo CAR T developers. Beyond early proof-of-concept, well-designed, GCP-compliant IITs generate rigorous safety, efficacy, and translational data that validate technology platforms and strengthen pipeline credibility. These studies produce integrated data packages—spanning preclinical rationale, CMC readiness, dose rationale, and clinical observations.
“Findings from IIT studies also generate critical data packages to support IND filings, and other regulatory milestones,” says Huiyi Zhu, head of U.S. project management at ProBio. “Importantly, these results can significantly enhance a cell and gene therapy (CGT) company’s position in securing funding, advancing toward an IPO, or negotiating out-licensing agreements.
The financial advantages are equally compelling. “By enabling the execution of high-quality, GCP-compliant clinical studies at less than half of the cost of a comparable U.S. trial, an IIT study also preserves a CGT company’s capital for key development priorities,” Zhu says. “We believe IIT will be an important regulatory pathway to enable and accelerate in vivo CAR T technology and pipeline development.”

Explore More www.probiocdmo.com/webinars/gene-cell-therapy-categories.