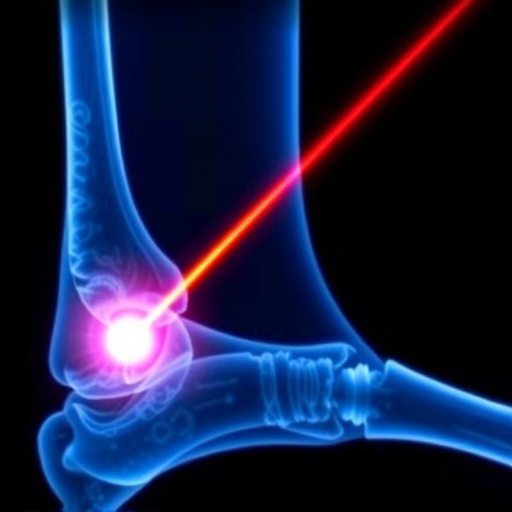
In the realm of surgical innovation, lasers have long been heralded for their precision and non-contact capabilities, making them ideal for delicate procedures. However, when it comes to operating on hard tissues such as bone, their application has been limited due to slow processing speeds and insufficient cutting depth. A pioneering study led by researchers at the University of Basel has now fundamentally shifted these limitations, demonstrating that by redefining the energy distribution within the laser beam, it is possible to significantly enhance both the depth and speed of bone cuts—ushering in a potential new era for bone surgery.
Traditional methods for cutting bone—saws, chisels, and drills—have been the substrates of orthopedic surgery for decades, valued for their reliability and effectiveness. Yet, these mechanical tools exert physical pressures that sometimes result in microcracks and less precise incisions. Lasers, in contrast, operate without mechanical force, offering the potential for more nuanced cuts with reduced collateral damage. This characteristic is especially promising for procedures involving the insertion of joint implants, which increasingly rely on custom, 3D-printed components that demand highly accurate bone preparation.
While lasers have become a mainstay in soft tissue surgeries, their effectiveness in bone has been curtailed by technical constraints. Previous laser systems could only achieve cut depths of approximately 2 to 3 centimeters, a range insufficient for many orthopedic applications, including joint replacements. A critical bottleneck was identified in the laser beam’s energy profile—the spatial distribution of energy that determines how efficiently material is ablated during cutting.
The breakthrough came through reengineering the laser beam’s intensity profile itself. Most conventional surgical lasers exhibit a Gaussian energy pattern: highest intensity at the core tapering off gradually toward the edges, resembling a flashlight beam or a bell-shaped curve. This uneven distribution means that a significant portion of the beam’s energy dissipates prematurely, limiting the effective cutting depth. The team, led by Dr. Ferda Canbaz from the University of Basel’s Department of Biomedical Engineering, introduced a novel “top hat” energy profile. This configuration distributes laser energy evenly across the beam’s cross-section before it sharply falls off at the edges, maximizing the energy utilization on the bone surface.
Experimentation with this modified beam on bovine bones yielded remarkable results. The laser equipped with the traditional Gaussian profile managed to cut only around 2.6 centimeters deep. By contrast, the top hat profile nearly doubled the cutting depth, achieving cuts up to 4.4 centimeters. This substantial increase not only surpasses prior cutting benchmarks but also edges closer to the depths required for clinical application in joint implant surgeries.
A key insight from the study is the manner in which energy is absorbed during the ablation process. In Gaussian laser beams, the uneven intensity leads to the walls of the cut absorbing substantial energy, progressively starving the bottom of the incision of sufficient power to proceed deeper. The top hat profile rectifies this by delivering an even energy distribution that minimizes losses to the incision walls, thereby maintaining cutting power at greater depths and enhancing efficiency.
Despite this progress, laser cutting still lags behind mechanical tools in terms of speed. The laser in its current iteration removes approximately 0.4 cubic millimeters of bone per second, whereas a conventional saw removes around 11 cubic millimeters—over twenty times as much volume in the same timeframe. Nevertheless, the enhanced depth performance is a critical step forward. The researchers emphasize that this innovation solves a ceiling effect on cut depth, not the speed limitation, marking a foundational advancement for future development.
Looking ahead, the team plans to refine the laser system further, focusing on augmenting both speed and cutting depth. Optimizing parameters such as beam modulation, pulse duration, and cooling techniques are essential to make the laser practical for routine clinical use. Moreover, adapting the laser for the complex and sensitive environment inside the human body presents additional challenges—particularly in safeguarding surrounding soft tissues while maximizing bone ablation.
Thermal management during cutting is another crucial technical consideration. Excessive heat can damage bone and hinder postoperative healing. To address this, the researchers applied continuous cooling using compressed air and water sprays to maintain lower temperatures and preserve tissue integrity during the cutting process. This approach not only prevents charring but also ensures that the precision of the cut is maintained by clearing debris efficiently.
The implications of this research stretch beyond orthopedic surgery. Precise laser osteotomy could eventually facilitate minimally invasive procedures, reduce recovery times, and enable the use of patient-specific implants with unparalleled precision. With increasing demand for personalized medicine and surgical accuracy, the advent of laser technology capable of deep bone ablation could transform surgical paradigms.
This project is rooted in the “Miracle” initiative, an enterprise aimed at developing cutting-edge technologies for bone surgery, generously supported by the Werner Siemens Foundation. Synergies with industrial partners, notably through the Innosuisse “Laser-Blade” project in collaboration with Smith&Nephew, a leading medical technology firm, underscore the translational potential of this innovation from bench to bedside.
In summary, the recalibration of surgical laser energy profiles from Gaussian to top hat represents a monumental stride in bone surgery. While speed remains a hurdle, achieving nearly double the cutting depth of previous laser systems opens new horizons for the role of lasers in orthopedics. As ongoing research addresses the remaining challenges of efficiency and clinical adaptation, surgical lasers may soon become indispensable instruments in operating theaters worldwide.
Subject of Research: Influence of laser beam intensity profile on deep bone ablation in laser osteotomy
Article Title: Influence of laser beam intensity profile on deep bone ablation in laser osteotomy
Web References: DOI: 10.1038/s41598-026-37117-6
Image Credits: University of Basel, Catherine Weyer
Keywords
Laser osteotomy, bone surgery, laser beam profiling, surgical laser, top hat beam, Gaussian beam, bone ablation, biomedical engineering, orthopedic surgery, cutting depth, laser efficiency, thermal management, laser cutting speed
Tags: 3D-printed joint implant preparationadvanced surgical laser energy distributionenhanced laser penetration in bonefaster bone cutting methodshigh-precision bone cutting laserslaser bone surgery innovationmicrocrack prevention in bone surgerynon-contact bone surgery techniquesorthopedic laser cutting technologyreducing collateral damage in bone surgeryreplacing mechanical bone cutting toolsUniversity of Basel laser research