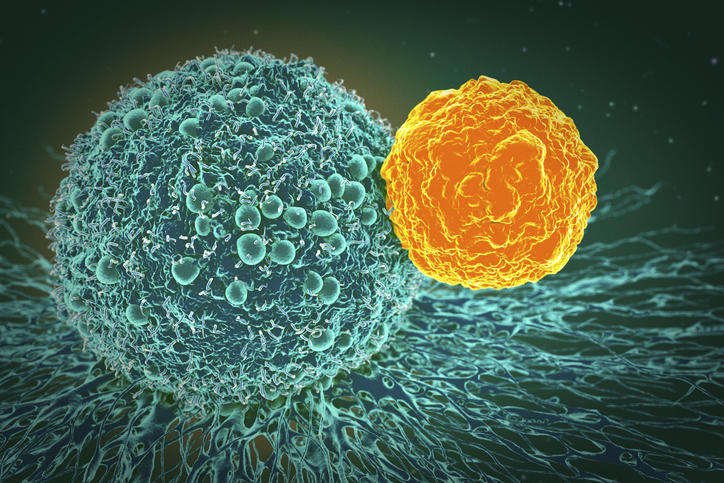
Chimeric antigen receptor (CAR) T-cell therapy is an impactful treatment for blood cancers, such as leukemia and lymphoma. However, the immunotherapy has struggled against solid tumors, as tumor cells often do not share one consistent surface target. Additionally, many solid tumors are protected by a dense network of scar tissue and immune-suppressive cells that block T-cells.
To address these challenges, researchers from Memorial Sloan Kettering (MSK) Cancer Center have developed a new CAR T-cell that attacks supportive cells in the tumor microenvironment that bear the surface protein, urokinase plasminogen activator receptor (uPAR). The work is described in a new study published in Cell titled, “A convergent uPAR-positive tumor ecosystem creates broad vulnerability to CAR T-cell therapy.”
Results showed that uPAR was elevated in 12 of the 14 human cancer types analyzed by the study. High uPAR expression was most strongly associated with mutations that compromise p53, the tumor-suppressor often called the ‘guardian of the genome,’ and activating mutations in KRAS and other genes in the RAS pathway. Additionally, strong uPAR levels were associated with the activation of genes that are important for cellular plasticity, inflammation, and fibrosis, which are all hallmarks of aggressive cancer.
Scott Lowe, PhD, chair of the cancer biology and genetics program at MSK and co-corresponding author of the study, emphasized that the new uPAR targeting approach shrank several types of solid tumor in the lab, including lung, pancreatic, and ovarian cancers and even cleared metastases in some experiments. These engineered cells selectively eliminated solid tumor cells, and fibroblasts and immunosuppressive myeloid cells that provide a protective environment for tumor growth.
The team tested the effectiveness of the uPAR-targeted CAR T cells in a range of preclinical systems, including cancer cells, human tumors grown in mice, and mouse models that mimic metastatic disease. Therapeutic effect was further enhanced when combined with senescence-inducing treatments, such as the chemotherapy agent cisplatin.
In a mouse model of ovarian cancer, uPAR-targeting CAR T cells led to durable remissions. Mice whose tumors had been eliminated also resisted developing new tumors, indicating that the CAR T cells remained active. Additionally, a single adjuvant dose of the engineered cells after surgery eliminated residual disease in mice. In contrast, surgery alone provided only temporary therapeutic effects.
By focusing on uPAR, the new approach allows researchers to target cells in a particular state rather than a specific type of cell. The findings support recent work from MSK showing that even when such cells represent only a subpopulation of the tumor, their elimination can lead to tumor collapse, and highlighting the functional importance of these specialized cell states.
Beyond CAR T cells, uPAR can be targeted with antibody–drug conjugates (ADCs), antibody-delivered radiation, and CAR-based natural killer cell treatments. The researchers also showed two potential approaches to monitor uPAR-high disease without a biopsy: measuring suPAR (a soluble fragment of uPAR) in blood, and using uPAR-targeted PET scans to identify tumors and metastases and track cancer treatment response over time.