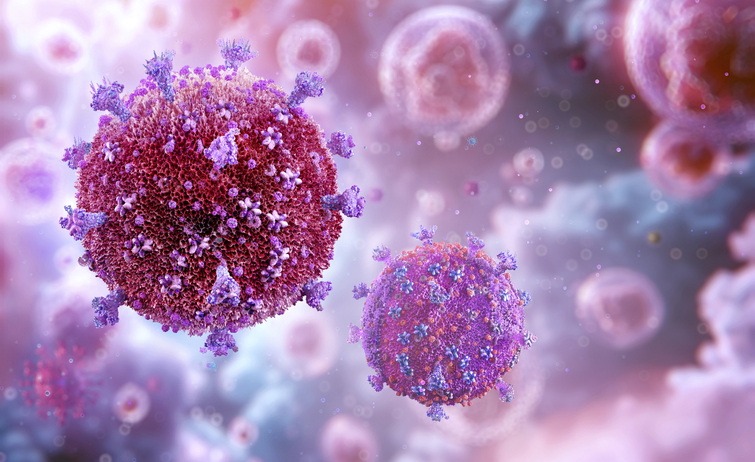
For millions of people with HIV (PWH), a daily regimen of medications is a lifelong necessity. If they stop taking antiretroviral therapy (ART), the virus usually rushes back within weeks.
But this isn’t the case for everyone. Scientists have been baffled by rare individuals who, after stopping the drug regimen, still keep the virus under control for months or even years. “Strikingly, a small number of people rebound much more slowly and take multiple months or even longer to rebound,” said Nadia Roan, PhD, senior investigator at Gladstone Institutes.
Studies by Roan and her team have now started to reveal why that is. Among the key findings, the team discovered two specific genes inside infected cells that act like security locks to keep the virus asleep. And perhaps most significantly, they also found that a common diabetes drug, metformin, can activate one of these locks to keep the virus in its dormant state. The results could point to potential new paths toward long-term health for people living with HIV, without the need for antiretroviral therapy.
“Our data suggest metformin might be able to delay, or possibly even prevent HIV rebound in some individuals, which is exciting because it’s a very safe and affordable drug,” said Roan. “We are now very interested in pushing forward with preclinical and eventually clinical studies to directly test these potential benefits.” Roan is senior author of the team’s published paper in Immunity, titled “Multiomic analysis of ART-interruption cohorts identifies cell-extrinsic and -intrinsic mechanisms driving lymphocyte-mediated control of HIV rebound.”
For people with HIV, antiretroviral therapy successfully controls the virus, but “reservoirs” of immune cells containing a permanent copy of HIV’s genetic code persist. “Antiretroviral therapy (ART) has been transformative for people with HIV (PWH) but is not curative as it cannot eliminate the long-lived reservoir of HIV-infected cells,” the authors wrote. If treatment is disrupted, this genetic code typically begins to generate active HIV, leading to a return of symptoms and, if left untreated, to acquired immunodeficiency syndrome (AIDS). “For most PWH, viremia typically rebounds within a period of a few weeks upon ART cessation.”
Rarely, people exhibit delayed rebound after ART withdrawal, and some, known as post-treatment controllers (PTCs), may stay in viral remission for months or even years after stopping ART. By studying these rare individuals who continue to suppress the virus even after treatment ends, Roan and her team sought to pinpoint features of immune cells that can keep the virus locked down.
![A team of Gladstone scientists—including Ashley George (left) and Nadia Roan (right)—uncovered a new path toward life without daily HIV pills, suggesting that a common diabetes pill could help achieve long-term remission. [Michael Short/Gladstone Institutes]](https://www.genengnews.com/wp-content/uploads/2026/03/Low-Res_Gladstone_AAA5023-300x169.jpg)
They turned to four recently completed clinical trials in which people with HIV deliberately went off treatment—underwent analytical treatment interruption (ATI)—in some cases to test potential HIV cures, and were carefully monitored for HIV rebound, at which time the individuals restarted antiretroviral therapy. “Our goal was to leverage a variety of ‘omics’ tools to identify host immune responses that associate with viral rebound time upon ART cessation, and to relate these findings to HIV persistence measurements, using specimens from four recent ATI trials,” the team stated.
Roan’s group obtained blood specimens taken from 75 trial participants immediately before they paused therapy, and measured levels of genes and proteins within multiple types of immune cells from the samples to uncover associations between these features and how long it took for HIV to rebound. These efforts yielded several important discoveries. In two of the trials, delayed rebound was associated with higher levels of a specific type of immune cell known as stem cell memory CD8+ T cells. In fact, the two patients with the most extremely delayed rebound—more than 22 weeks for one and over 33 weeks for the other—also had the highest levels of these cells.
“These CD8+ T cells appear to have ‘stem-like’ features and might be able to stick around to continue replenishing themselves for prolonged periods of time, which may help them contribute to long periods of ART-free HIV control,” Roan said.
In another trial, people with an atypical type of natural killer cells rebounded later than patients with the conventional version. Natural killer cells are a type of immune cell typically thought of as destroyers of virus-infected cells. But they can also help regulate how other immune cells operate, which may impact post-therapy HIV rebound.
“All together, our findings suggest there’s probably not just one solution for suppressing HIV,” commented co-author Ashley George, PhD, research scientist at Gladstone and co-first author on the study. “By leveraging different features of immune cells that can help fight infection, we likely have multiple opportunities to control HIV without the need for ART.”
The study’s most striking findings came from some of the patients’ CD4+ T cells—the main cell type that serves as a reservoir for HIV. People whose reservoir cells had higher levels of two particular genes, DDIT4 and ZNF254, tended to have longer HIV rebound times after stopping antiretroviral therapy. In follow-up lab experiments, Roan and her team confirmed that both genes can suppress HIV.
George added, “Both genes represent possible new targets for a promising ‘block and lock’ strategy for curing HIV, in which drugs would first be used to block HIV activation, followed by ways to make this block permanent.”
This approach is a major focus of the HIV Obstruction by Programmed Epigenetics (HOPE) Collaboratory, a multidisciplinary group of researchers, including Roan and other co-authors on the new study, working toward an HIV cure. When the scientists further analyzed publicly available data, they uncovered more supporting evidence. They found that people with higher levels of the two genes had reduced HIV activity in their cells. And, in “elite controllers”—people whose bodies naturally suppress HIV from the start of infection, even without therapy—levels of the gene ZNF254 among CD4+ T cells are much higher. “One possibility we’re imagining for the future is that we could somehow deliver ZNF254 to infected cells in order to turn people into elite controllers,” George said. “We could also try to engineer an even stronger version of this gene.”
But of all findings in the new study, the link between gene DDIT4 and delayed rebound may have the most immediate ramifications for patients. That’s because levels of this gene can be boosted by the drug metformin—something that had already been observed by the scientific community in non-immune cells, and which this study demonstrated is also true in T cells.
This led the scientists to conduct a series of experiments to validate whether metformin can help suppress HIV. In one notable experiment, treating cells taken from people with HIV with metformin blocked the ability of HIV to reactivate, suggesting a possible role for this drug in helping achieve “block and lock.” In their paper, they stated, “Metformin induced DDIT4 and suppressed HIV expression in primary cells and cells from ART-suppressed PWH, suggesting that this affordable diabetes drug could be repurposed to silence HIV. Our results support the pursuit of both immune- and HIV-silencing strategies to achieve ART-free HIV remission.” Next, the team is planning to test metformin and related compounds in a variety of preclinical models for their ability to prevent HIV reservoir cells from generating active HIV upon interruption of antiretroviral treatment.
“Future studies should examine the extent to which DDIT4 and ZNF254 can mediate post-ATI control in other cohorts, and test the therapeutic potential of targeting the pathways associated with these genes,” the team stated. “For example, we propose the implementation of a placebo-controlled ATI trial testing the effects of metformin treatment both during ART and post ATI,” they further wrote.
Drugs that effectively silence HIV could also have health benefits even for those who stay on antiretroviral therapy. This is because the drugs can limit the levels of viral gene products—a driver of inflammation—that these individuals are chronically exposed to.
“We are excited to pursue HIV silencing strategies both as a way to achieve block and lock, but also as a strategy to improve the overall health of people with HIV by lessening chronic inflammation,” Roan said.