In an era where precision in pediatric diagnostics can radically alter clinical outcomes, the advent of enhanced imaging techniques has paved the way for groundbreaking advancements in detecting severe respiratory conditions. A recent study published in Pediatric Research unveils the compelling potential of lung ultrasound (LUS) as a diagnostic tool in identifying lung necrosis among children afflicted with community-acquired pneumonia (CAP). This revelation emerges as a beacon of hope in pediatric care, offering a non-invasive, radiation-free alternative to conventional diagnostic modalities.
Community-acquired pneumonia remains a significant cause of morbidity and mortality in children worldwide, with complications such as lung necrosis posing substantial treatment challenges. Lung necrosis, characterized by the death of lung tissue due to severe infection and inflammation, often requires prompt and accurate diagnosis to guide therapeutic strategies, including surgical intervention, antibiotics, and supportive care. Historically, computed tomography (CT) has been the gold standard for detecting lung necrosis, but its use is limited by radiation exposure, costs, and the need for sedation in young patients.
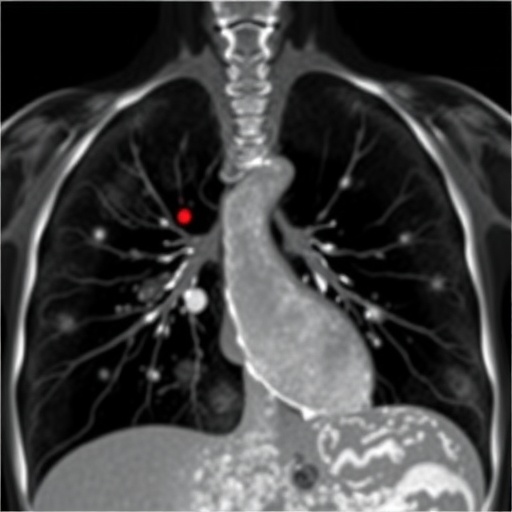
The recent investigation delves into the diagnostic performance of lung ultrasound in this context, analyzing its sensitivity, specificity, and overall reliability compared to CT imaging. Lung ultrasound offers a radiation-free, bedside imaging technique capable of real-time visualization of pulmonary structures, making it particularly suitable for pediatric populations who are more vulnerable to ionizing radiation risks. The study’s methodology involved a cohort of pediatric patients presenting with community-acquired pneumonia, undergoing both LUS and CT scans to ascertain the presence or absence of lung necrosis.
Intricately, lung ultrasound leverages sonographic principles to detect changes in lung parenchyma and pleural surfaces associated with necrotic tissue, such as subpleural consolidations, hypoechoic regions indicative of cavitation, and irregular air bronchograms. The researchers meticulously identified sonographic markers correlating with necrotic areas, establishing a framework for standardized LUS interpretation in this clinical scenario. This methodological advancement is vital, given the operator-dependent nature of ultrasound imaging and the necessity for reproducible diagnostic criteria.
The results herald a paradigm shift in pediatric respiratory diagnostics. Lung ultrasound demonstrated high diagnostic accuracy, with sensitivity and specificity metrics approaching those of CT scans, underscoring its efficacy as a frontline imaging tool. These findings carry profound implications, suggesting that lung ultrasound can not only expedite diagnosis but also reduce reliance on CT imaging, thereby minimizing radiation exposure and healthcare costs. The bedside applicability of LUS further enhances its clinical utility, enabling prompt decision-making in acute settings.
Beyond its diagnostic prowess, lung ultrasound offers dynamic monitoring capabilities. Unlike static CT scans, LUS can be repeated as frequently as clinically indicated, providing clinicians with a real-time window into disease progression or resolution. This feature is particularly advantageous in managing complicated pneumonia cases, where therapeutic responses must be closely surveilled to tailor interventions effectively and avoid complications such as abscess formation or bronchopleural fistula.
The study also highlights the learning curve and resource implications associated with widespread adoption of lung ultrasound. While the technology is increasingly available, its successful integration into routine practice hinges on operator proficiency, requiring comprehensive training and credentialing. The researchers advocate for standardized educational protocols and multidisciplinary collaboration to harness the full potential of LUS, emphasizing that technological advances must be complemented by human expertise for optimal patient outcomes.
Importantly, this research aligns with the broader shift towards precision medicine in pediatric care, where individualized, minimally invasive diagnostics guide targeted therapies. By facilitating early and accurate detection of lung necrosis, lung ultrasound empowers clinicians to stratify patients based on disease severity and tailor treatment regimens accordingly, potentially reducing hospital stays, complications, and long-term sequelae.
The implications of these findings extend into public health domains as well. In resource-limited settings where access to CT is restricted or unavailable, lung ultrasound emerges as a pragmatic tool, democratizing high-quality care for vulnerable pediatric populations. Its portability and cost-effectiveness make it an ideal candidate for integration into frontline healthcare services, mitigating disparities in diagnostic capabilities globally.
Furthermore, lung ultrasound’s role in augmenting pediatric respiratory diagnostics may spur technological innovation. Enhanced ultrasound devices equipped with automated pattern recognition and artificial intelligence algorithms could streamline image interpretation, reduce inter-operator variability, and further improve diagnostic accuracy. This convergence of imaging and computational advances epitomizes the future direction of medical diagnostics.
The findings also prompt a reevaluation of clinical guidelines concerning pneumonia management. Integrating lung ultrasound into diagnostic algorithms could redefine standard care pathways, prioritizing ultrasound evaluation in initial assessments and follow-up. Such updates would need to be underpinned by robust evidence, multidisciplinary consensus, and ongoing research to optimize protocols and validate outcomes across diverse patient populations.
In conclusion, the study published in Pediatric Research illuminates the transformative potential of lung ultrasound for detecting lung necrosis in children with community-acquired pneumonia. By offering a non-invasive, accurate, and accessible diagnostic modality, LUS stands poised to reshape pediatric respiratory care, enhancing patient safety, reducing costs, and improving clinical outcomes. The journey towards widespread adoption necessitates concerted efforts in education, infrastructure, and research, yet the clinical and societal benefits underscore a compelling case for embracing this technology.
As the medical community continues to grapple with optimizing diagnostics for vulnerable pediatric cohorts, lung ultrasound offers a tangible, effective solution aligned with modern healthcare imperatives. It exemplifies how innovation, when thoughtfully applied, can bridge gaps in care, reduce harm, and elevate standards of pediatric medicine on a global scale.
Subject of Research: Lung ultrasound in diagnosing lung necrosis in pediatric community-acquired pneumonia
Article Title: Diagnostic performance of lung ultrasound for detecting lung necrosis in children with community-acquired pneumonia
Article References:
Elmeazawy, R., AbdElsamea, M.Z., Elaskary, E.M. et al. Diagnostic performance of lung ultrasound for detecting lung necrosis in children with community-acquired pneumonia. Pediatr Res (2026). https://doi.org/10.1038/s41390-026-05026-z
Image Credits: AI Generated
DOI: 06 May 2026
Keywords: Lung ultrasound, lung necrosis, community-acquired pneumonia, pediatric diagnostics, imaging, pediatric pneumonia, non-invasive imaging, CT alternative, pediatric respiratory care
Tags: advantages of lung ultrasound in pediatricsbedside imaging for respiratory conditionscommunity-acquired pneumonia complicationsdetecting lung necrosis with ultrasoundlung necrosis identification in childrenlung ultrasound in pediatric pneumonianon-invasive pneumonia diagnosis in childrenpediatric lung imaging techniquespediatric pneumonia treatment strategiesradiation-free pediatric diagnostic toolsreal-time lung ultrasound diagnosticsultrasound vs CT in lung necrosis