A recent comprehensive investigation spearheaded by researchers at the University of Nottingham has unveiled critical socio-economic disparities affecting access to mental health services among children and young people grappling with emotional and psychological challenges. This pivotal research, published in The British Journal of Psychiatry, sheds light on systemic inequities within child and adolescent mental health services (CAMHS) that disproportionately disadvantage individuals from deprived neighborhoods, leading to a troubling cycle of unmet needs and poor long-term outcomes.
The study undertook an extensive prospective longitudinal analysis, drawing upon data obtained from the STADIA trial—a large-scale, multicenter randomized controlled trial encompassing eight major NHS Trusts across England. This cohort included 1,225 children and young people referred to CAMHS due to emotional difficulties such as anxiety and depression. Over the course of 18 months, participants were monitored to assess service engagement, clinical diagnoses, and symptom trajectories, enabling researchers to scrutinize patterns of referral acceptance and treatment efficacy within different socio-economic groups.
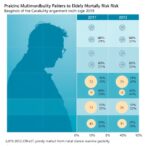
What emerged from this rigorous data analysis was a clear and sobering narrative: children and young people residing in the most socio-economically deprived areas were considerably less likely to have their referrals to CAMHS accepted. Those from these communities not only faced greater rejection rates but also demonstrated poorer clinical outcomes even after one year of follow-up. This reveals a significant inequity in both access to and the quality of mental health care, suggesting that systemic barriers may impede early intervention efforts critical to altering the course of mental health trajectories in young populations.
Age also surfaced as a crucial factor influencing service receipt. Notably, children under the age of eleven were less likely to receive mental health support post-referral. This gap is particularly alarming given the importance of timely intervention in childhood for ameliorating mental health conditions and preventing their escalation into chronic disorders. The data imply structural deficiencies in how younger children’s mental health issues are recognized and addressed, compounding their vulnerability within an already strained system.
The longitudinal data reveal a disheartening reality regarding treatment outcomes. A striking 61% of those referred continued to meet criteria indicating the need for ongoing mental health support one year later. This stagnation underscores substantial challenges in the effectiveness of current care models and indicates that the majority of children receiving services do not achieve sufficient clinical improvement. Numerous factors may contribute to this plateau, including insufficient resource allocation, inadequate tailoring of interventions to individual needs, and delayed access to services.
Professor Kapil Sayal, Chief Investigator and a leading figure at the University of Nottingham’s School of Medicine, highlighted the alarming escalation in mental health problems among young people over recent years. He emphasized the mismatch between increasing prevalence and the capacity of services, necessitating triage and prioritization protocols that, while pragmatic, may inadvertently marginalize vulnerable groups. The study’s findings call for urgent reevaluation of these systemic processes to ensure equitable and timely access to care.
In the broader context, the mental health of children and adolescents has emerged as a formidable public health challenge internationally, with emotional disorders such as anxiety and depression showing marked increases, particularly catalyzed by the repercussions of the COVID-19 pandemic. Heightened symptom severity and escalated help-seeking behavior have strained existing health infrastructures globally. Nevertheless, this study articulates an unsettling truth: despite recognition of rising demand, access to evidence-based interventions remains grossly insufficient and unevenly distributed.
The research methodology leveraged robust statistical data analysis to disentangle the complex interplay between socio-economic status, age, service acceptance, and clinical efficacy. By systematically following a large, diverse, and nationally representative population cohort, the study offers compelling empirical evidence of entrenched health inequalities. It also enables a nuanced understanding of who is more likely to be seen within the system, who receives meaningful support, and crucially, who improves as a result of intervention.
Findings from this study have major implications for policymakers, clinicians, and service providers alike. The identification of significant disparities in service access and outcomes calls for the urgent development of equitable mental health service models that prioritize inclusivity and early intervention. There is a clear mandate to redesign referral pathways, enhance resource allocation to underserved areas, and create interventions that are both culturally sensitive and developmentally appropriate.
Moreover, the persistence of unmet clinical needs indicates the necessity of innovation within treatment paradigms. Collaborative, multi-disciplinary approaches and increased integration between education, social services, and healthcare may prove essential to bridging existing service gaps and optimizing recovery trajectories. Embedding flexible, community-based supports could better accommodate the diverse circumstances of children and young people from disadvantaged backgrounds.
This study also intersects with ongoing governmental and health authority efforts to reform mental health services. The Department of Health and Social Care (DHSC) is currently conducting an independent review into mental health conditions, underscoring the timeliness and relevance of these findings. Integrating insights from empirical research such as STADIA can help inform evidence-based policy reforms and funding decisions that aim to close the mental health inequality gap.
In sum, the University of Nottingham-led investigation provides a landmark contribution to understanding how socio-economic deprivation critically shapes mental health service trajectories and outcomes among young people. It paints a compelling picture of systemic challenges that hinder equitable healthcare delivery in one of the most vulnerable populations. Addressing these disparities is not only a moral imperative but a public health necessity, bearing profound implications for social justice and the future well-being of upcoming generations.
The STADIA trial’s data-driven lens elucidates a complex but actionable pathway forward: reforming referral systems, prioritizing early and equitable intervention, and innovating care models to ensure sustained clinical improvement. As mental health disorders among children and young people continue to rise globally, there is a pressing need for health systems to adapt quickly—ensuring no child’s mental health is left behind due to socio-economic circumstance or developmental stage.
Subject of Research: People
Article Title: Investigating inequalities in children and young people’s mental healthcare and outcomes: prospective longitudinal analysis from the STADIA trial
News Publication Date: 27-Apr-2026
Web References: http://dx.doi.org/10.1192/bjp.2026.10617
Keywords: Mental health, Children, Young people, Socio-economic inequalities, Child and adolescent mental health services, Access to care, Clinical outcomes, Emotional disorders, Anxiety, Depression, Early intervention, Health disparities
Tags: access to adolescent mental health careanxiety and depression in socioeconomically disadvantaged childrenbarriers to child mental health servicesCAMHS referral rejection rateschild and adolescent emotional difficultiesimpact of poverty on mental health treatmentlong-term outcomes of unmet mental health needslongitudinal study on mental health accessmental health inequities in deprived areasmental health service engagement in youthNHS mental health service accessibilitysocioeconomic disparities in mental health