Keratoconus, a debilitating eye condition characterized by progressive thinning and deformation of the cornea, poses significant diagnostic challenges, especially in its earliest stages. While conventional diagnostic tools rely heavily on corneal shape and thickness, these parameters often fail to capture subtle, preclinical tissue changes that herald disease progression. Recent advancements in imaging technology, however, promise to bridge this diagnostic gap. In a groundbreaking study published in Biophotonics Discovery, researchers unveiled a novel approach that integrates polarization-sensitive optical coherence tomography (PS-OCT) with artificial intelligence (AI) algorithms to detect early microstructural alterations in the cornea, potentially revolutionizing subclinical keratoconus diagnosis.
Most traditional screening technologies—including Pentacam and MS-39—depend on assessing macroscopic features such as corneal curvature, thickness, and surface irregularities. These metrics, while efficacious for diagnosing established keratoconus, often fall short when the disease is nascent and changes remain microscopic. During these early phases, the cornea may outwardly appear normal under routine clinical examination, obscuring internal disruptions within its collagen matrix. Recognizing this limitation, the study authors shifted focus toward detecting subtle collagen fiber disorganization—an early hallmark of keratoconus that precedes conspicuous shape distortion.
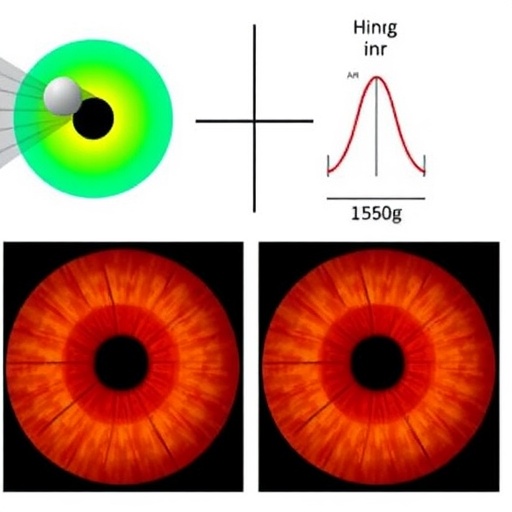
PS-OCT, an advanced imaging modality, exploits the interaction between polarized light and biological tissues to reveal microstructural organization inaccessible to conventional tomography. When polarized light traverses the cornea, its retardation—alterations in polarization state—encodes information about the alignment and integrity of collagen fibrils, which are vital for maintaining corneal biomechanical strength and transparency. This method offers ultrahigh resolution and the capacity to generate phase retardation maps that reflect collagen orientation with remarkable sensitivity.
Leveraging a bespoke PS-OCT instrument, the researchers collected comprehensive corneal datasets from 359 eyes, encompassing healthy individuals, clinically diagnosed keratoconus patients, and a substantial cohort exhibiting subclinical keratoconus. The device’s imaging capabilities allowed detailed layer-specific measurements, including epithelium, Bowman’s layer, and stroma thickness, alongside multifaceted polarization data crucial for discerning microarchitectural differences.
To objectively evaluate diagnostic performance, the research team implemented three independent AI models corresponding to data derived from PS-OCT, Pentacam, and MS-39, respectively. Utilizing identical machine learning frameworks and validation techniques ensured fair comparison across modalities. While accuracy rates were comparable for unequivocally healthy or diseased eyes, distinct disparities emerged when evaluating subclinical cases. The PS-OCT-driven AI demonstrated a unique ability to reclassify certain eyes previously deemed subclinical by tomography as truly healthy based on collagen organization patterns, effectively reducing false-positive diagnoses.
This strategic reclassification hinged not on arbitrary distinctions but on substantial biophysical evidence. Eyes labeled subclinical by PS-OCT exhibited increased phase retardation and detectable thinning of Bowman’s layer, even absent conspicuous corneal shape anomalies. Conversely, eyes reverted to healthy classification revealed collagen and layer thickness consistent with normal corneal integrity, underscoring the technique’s specificity and nuanced diagnostic capability.
Visual inspection of phase retardation maps furnished compelling insights. Healthy corneas displayed homogenous retardation signals indicative of well-aligned collagen fibers and symmetrical Bowman’s layer thickness. In contrast, subclinical keratoconus samples presented moderate but consistent central increases in phase retardation coupled with subtle Bowman’s layer thinning—suggesting early collagen remodeling. Established keratoconus cases revealed chaotic, irregular retardation distributions alongside marked morphological abnormalities, aligning with known disease pathology.
These findings hold profound clinical implications. Vis-à-vis patient management, a frequent conundrum arises when thin or marginally atypical corneas are categorized as “suspect,” prompting conservative intervention or denial of refractive surgeries. PS-OCT’s capacity to distinguish genuinely compromised tissue from naturally thin yet stable corneas heralds a paradigm shift, allowing ophthalmologists to tailor treatment strategies with increased confidence and potentially expanding surgical candidacy safely.
Moreover, PS-OCT’s integration with AI algorithms exemplifies the potency of combining sophisticated imaging with computational intelligence — enabling multidimensional analysis of corneal health beyond mere morphology. Such synergy not only enhances sensitivity but also circumvents subjective interpretation pitfalls, laying groundwork for standardizing early keratoconus detection robustly across diverse clinical settings.
While the current study establishes a promising new frontier, the authors emphasize necessity for prolonged longitudinal studies to validate whether PS-OCT-based reclassifications accurately predict disease stability or progression over extended periods. Nonetheless, immediate utility for screening and diagnostic refinement is evident, particularly in refractive surgery candidate evaluation programs where early differentiation between pathological and physiological corneal features is critical.
Looking ahead, this research epitomizes a broader trend within biomedical optics: harnessing polarization-sensitive imaging to unlock deeper tissue characterization, which traditional intensity-based modalities overlook. Future technological innovations might further amplify resolution and data richness, integrating seamlessly with AI advances to personalize ocular healthcare, monitor corneal pathologies dynamically, and optimize treatment outcomes.
In conclusion, polarization-sensitive optical coherence tomography augmented by artificial intelligence represents a transformative leap in ophthalmic imaging. By illuminating microscopic organizational changes in corneal collagen, this technique bridges existing diagnostic gaps, facilitates earlier disease detection, and ultimately enhances clinical decision-making in keratoconus management. As this methodology gains traction, it promises to elevate corneal diagnostics from structural observation to functional tissue analysis, aligning perfectly with the era of precision medicine.
Subject of Research:
Optical imaging techniques for early keratoconus detection and artificial intelligence applications in ophthalmology.
Article Title:
Advancing subclinical keratoconus detection using polarization-sensitive optical coherence tomography and artificial intelligence.
News Publication Date:
9-Feb-2026
Web References:
https://www.spiedigitallibrary.org/journals/biophotonics-discovery/volume-3/issue-01/015004/Advancing-subclinical-keratoconus-detection-using-polarization-sensitive-optical-coherence-tomography/10.1117/1.BIOS.3.1.015004.full
References:
Patil, R. P., et al. “Advancing subclinical keratoconus detection using polarization-sensitive optical coherence tomography and artificial intelligence,” Biophotonics Discovery 3(1), 015004 (2026), doi:10.1117/1.BIOS.3.1.015004.
Image Credits:
R. P. Patil et al.
Keywords
Tomography, Eye, Optical Coherence Tomography, Polarization-sensitive Imaging, Keratoconus, Corneal Collagen, Artificial Intelligence, Biomedical Imaging, Ophthalmology, Corneal Microstructure, Bowman’s Layer, Refractive Surgery Screening
Tags: advanced imaging for keratoconusAI algorithms for corneal diseaseartificial intelligence in ophthalmologybiophotonics in ophthalmic diagnosticscorneal collagen fiber analysisearly detection of keratoconusearly-stage keratoconus screeningkeratoconus diagnosis with AImicrostructural corneal changespolarization-sensitive optical coherence tomographyPS-OCT in eye diseasesubclinical keratoconus detection