In a groundbreaking study poised to reshape our understanding of endometriosis, researchers at Washington State University have uncovered compelling evidence that the repeated cycle of inflammation characteristic of the disease does more than just damage pelvic tissues—it fundamentally rewires the brain’s pain processing mechanisms. This discovery not only elucidates longstanding mysteries about the disease’s debilitating pain but also opens transformative avenues for therapeutic intervention, challenging conventional approaches largely centered on lesion removal and hormonal suppression.
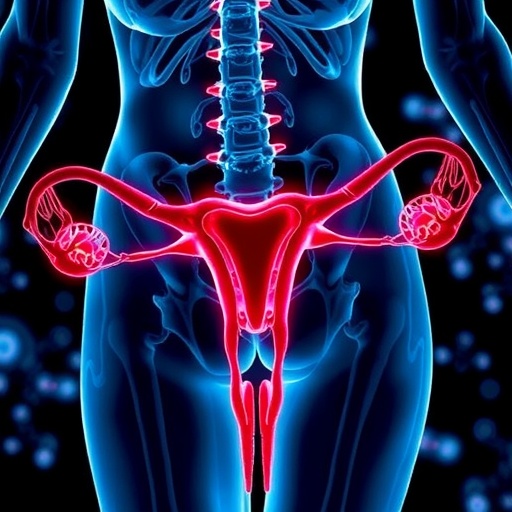
Endometriosis, a chronic gynecological condition where tissue similar to the uterine lining grows outside the uterus, afflicts approximately 10% of women of reproductive age—translating to about 190 million individuals worldwide. Traditionally, the severity of pelvic pain reported by patients often failed to correlate with the extent of visible lesions observed during medical examination, leaving researchers perplexed regarding the underlying cause of this disparity. The study led by Professor Kanako Hayashi, published in the Journal of Clinical Investigation, brings to light the crucial role of neuroinflammation and central nervous system sensitization triggered by recurrent inflammatory cycles typical of the menstrual process.
Hayashi’s team employed an innovative experimental model in mice designed to mimic the naturally occurring phenomenon of retrograde menstruation—where menstrual tissue flows backward into the pelvic cavity rather than exiting the body. Previous models only induced a single episode of this condition. However, by simulating multiple cycles, the study captured the cumulative impact of repeated inflammatory insults on the nervous system, revealing a progressive sensitization that amplifies and prolongs pain perception beyond the presence of physical lesions.
The neurobiological basis for this sensitization lies in the cascade of inflammatory signals originating in the pelvic region, which propagate through peripheral nerves to the spinal cord and ultimately to the brain’s pain-processing centers. Repeated stimulation results in neuroinflammation—a state characterized by the activation of glial cells and increased release of pro-inflammatory cytokines—thereby potentiating neuronal excitability. This central sensitization manifests as heightened sensitivity to pain stimuli, where even mild signals are perceived as intensely painful, creating a state of chronic pain independent of peripheral pathology.
Crucially, the study’s findings provide a mechanistic explanation for one of the most vexing clinical observations in endometriosis: why many patients continue experiencing severe pain long after surgical removal of lesions. This persistent pain arises because the sensitized central nervous system maintains an aberrant feedback loop. The brain, primed by neuroinflammation, perpetually reinforces pain signaling pathways back to the pelvis, effectively creating a self-sustaining cycle of pain that transcends the initial physical insult.
To validate the translational relevance of their animal model, the researchers collaborated with the Oregon National Primate Research Center to analyze tissue specimens from rhesus macaques naturally afflicted with endometriosis. These primate samples corroborated the mouse model findings, highlighting comparable neuroinflammatory changes associated with disease progression. This cross-species validation underscores the robustness of the study’s conclusions and the wider significance of central nervous system sensitization in endometriosis pathophysiology.
Beyond explicating disease mechanisms, this research pivotally suggests novel therapeutic targets. Treatments aimed solely at eliminating ectopic lesions or suppressing hormonal cycles have had limited success in alleviating pain for many patients. By contrast, compounds that modulate inflammation within the nervous system itself hold promise for breaking the vicious cycle of central sensitization. In the murine model, both a commonly prescribed hormonal therapy and an immunomodulatory agent attenuated pain sensitivity and diminished central neuroinflammation without necessarily reducing lesion size, pointing toward potentially paradigm-shifting pain management strategies.
Furthermore, this study establishes a comprehensive experimental system that allows real-time tracking of disease initiation through to the manifestation of chronic pain, offering researchers an invaluable tool to dissect the interplay of immune and nervous system components in endometriosis. Such a model paves the way for accelerated screening and development of targeted pharmaceuticals, potentially transforming clinical care by facilitating earlier diagnosis and more effective, personalized treatments.
Professor Hayashi emphasized that this research decisively reframes endometriosis as a multisystem disorder rather than a purely gynecological condition. “Our findings underscore that pain in endometriosis is not merely a symptom of local tissue damage but is fundamentally driven by the brain’s altered processing of pain signals, a persistent state of heightened neural sensitivity,” she explained. This insight demands that clinicians and researchers broaden their investigative and therapeutic vistas to encompass central neurobiological factors alongside peripheral disease manifestations.
The implications of this work resonate beyond endometriosis. Chronic pain conditions characterized by similar neuroimmune interactions—such as fibromyalgia and interstitial cystitis—may share underlying pathways of central sensitization. Hence, this study contributes to a growing body of evidence highlighting neuroinflammation as a critical driver in chronic pain syndromes, potentially inspiring cross-disciplinary research and therapeutic innovations.
As the scientific community continues to unravel the intricate mechanisms linking menstrual cycle–associated inflammation to chronic neurological changes, patients and clinicians gain new hope for alleviating the burden of endometriosis-associated pain. This research heralds a future where understanding and targeting the neural circuitry of pain could dramatically improve quality of life for millions worldwide afflicted by this enigmatic disease.
Subject of Research: chronic pain mechanisms in endometriosis involving neuroinflammation and central nervous system sensitization.
Article Title: Repeatedly occurring retrograde menstruation intensifies central sensitization driven by neuroinflammation in endometriosis models
News Publication Date: 17-Mar-2026
Web References: http://dx.doi.org/10.1172/JCI194136
References: Hayashi K, et al. Repeatedly occurring retrograde menstruation intensifies central sensitization driven by neuroinflammation in endometriosis models. Journal of Clinical Investigation. 2026.
Keywords: Endometriosis, neuroinflammation, central sensitization, chronic pain, retrograde menstruation, nervous system, pelvic pain, immunomodulation, hormonal therapy, neuroimmune interaction, pain hypersensitivity, gynecological disorders
Tags: brain rewiring pain processingcentral nervous system sensitization menstrual painchronic gynecological pain studieschronic pelvic pain mechanismsendometriosis brain pain connectionendometriosis inflammation cyclesendometriosis pain neurological changesinnovative endometriosis treatment researchneuroinflammation in endometriosisnon-hormonal endometriosis therapiespelvic tissue damage endometriosisretrograde menstruation experimental model